With applications for the new Bundled Payment for Care Improvement (BPCI) Advanced Model due March 12, the Centers for Medicare & Medicaid Services (CMS) released a new set of Frequently Asked Questions clarifying the application process and other topics. Medical group practices and hospitals are eligible to participate on their own, or with multiple entities under a convener.
Once the application is submitted, additional practices cannot be added. The model is set to begin Oct. 1, 2018. Qualifying Advanced Payment Model Participant determinations for the Medicare Quality Payment Program (QPP) will start in 2019 and vary by participant type, see below:
Bundled Payments for Care Improvement (BPCI) Advanced and Qualifying Advanced Payment Model Participant (QP) determinations
The first “snapshot” date for QP determination for eligible clinicians (ECs) following the start of BPCI Advanced will be March 31, 2019.
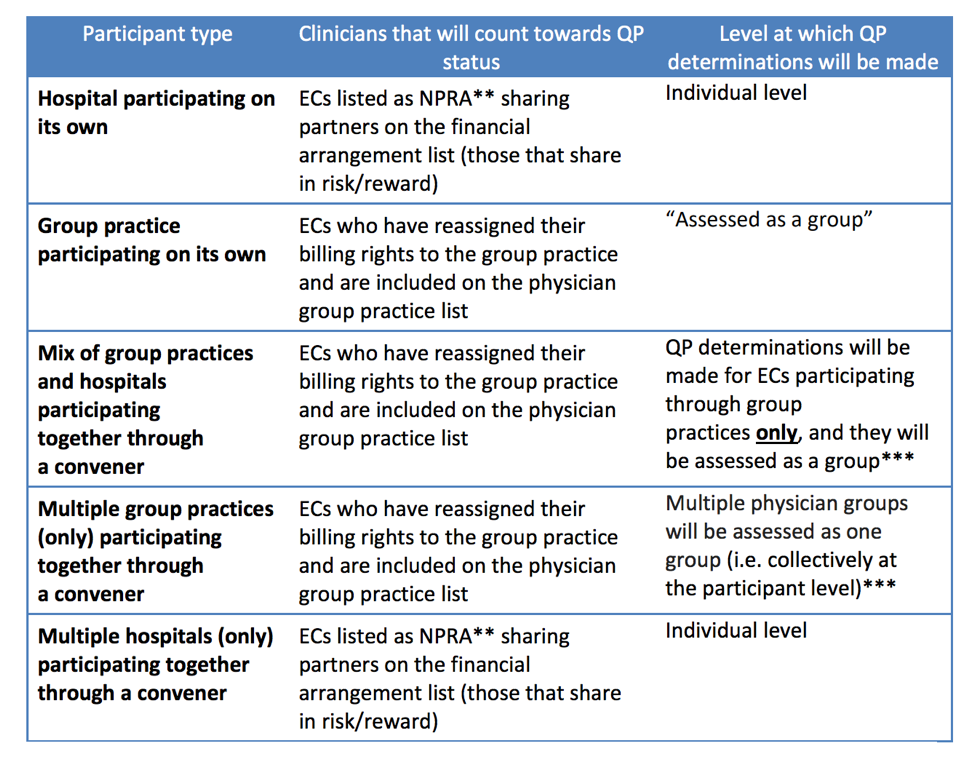
* Advanced APM ECs include physicians, physician assistants, nurse practitioners, clinical nurse specialists, certified registered nurse anesthetists, certified nurse-midwives, clinical social workers, clinical psychologists, registered dietitians or nutrition professionals, physical or occupational therapists, qualified speech-language pathologists, and qualified audiologists.
** NPRA = Net Payment Reconciliation Amount (final amount owed to or by a participant following reconciliation of actual spending against target spending)
*** A single convener can send in multiple applications and manage participants separately if group practices do not want to be assessed collectively or if hospital sharing partners want to qualify for QP status.
Courtesy of MGMA, March 8, 2018.





