Maximize the use of your EHR

Understanding Quality
Payment Programs (QPP)
Navigating the Quality Payment Program can feel overwhelming, especially as requirements and scoring rules continue to evolve. QPP affects how clinicians report data, how performance is measured, and ultimately how Medicare reimburses your practice.
Whether you’re evaluating MIPS participation, curious about Advanced APMs, or simply seeking clarity, we’ve gathered resources in our Learning Center to help you build confidence and stay informed.

Our Professional Services team is here to help.
Schedule a discovery call with one of our consultants to assess your needs and build a personalized strategy for success.
What is QPP?
The Quality Payment Program (QPP) helps Medicare providers transition from volume-based to value-based care through flexible reporting options and performance-based incentives.
MIPS: Merit-Based Incentive Payment System
MIPS is a program measuring an eligible clinician’s performance and comparing it with their peers. MIPS is a budget neutral program; the positive Medicare payments adjustments are funded by those receiving negative payment adjustments. The payments are applied to Medicare Part B payments for covered professional services two years after the performance period.
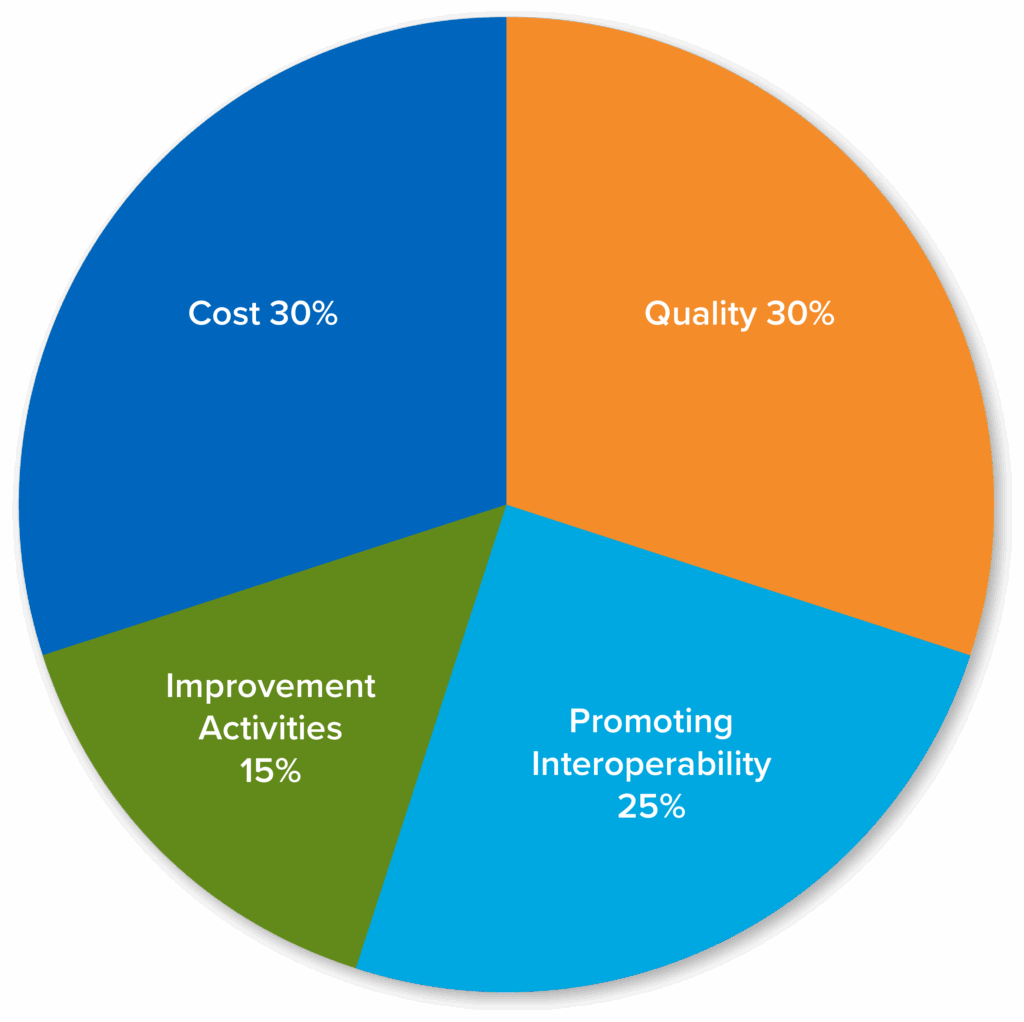
Performance Categories
Quality – 30% – 12 months
Cost – 30% – 12 months
Promoting Interoperability – 25% – 180 consecutive days
Improvement Activities – 15% – 90 consecutive days
Reporting Options
Traditional MIPS
MIPS Value Pathways (MVPs)
APM Performance Pathway (APP)
Scoring
Composite score (0–100)
Score ≥75 avoids penalties and may earn bonuses
MVPs: MIPS Value Pathways
MVPs offer a simplified, specialty-focused approach to MIPS reporting.
Why Choose MVPs?
- Pre-defined measure sets tailored to your specialty
- Subgroup reporting for multispecialty practices
- Includes foundational measures like Promoting Interoperability and population health
Transition Timeline:
- MVPs are optional through 2026
- CMS plans to phase out Traditional MIPS

MIPS vs. MVPs: Quick Comparison
Feature
Traditional MIPS
MVPs
Reporting Structure
Flexible but complex
Streamlined and specialty-focused
Measure Selection
Broad and manual
Pre-grouped by clinical relevance
Subgroup Reporting
Not supported
Supported
Relevance to Practice
May include unrelated measures
Specialty-aligned
Reporting Burden
Higher
Lower
Future Outlook
Being phased out
CMS-preferred model
Population Health Measures
Optional
Included

APMs: Alternative Payment Models
APMs reward providers for delivering high-quality, cost-efficient care.
Types of APMs:
- MIPS APMs – Hybrid models with MIPS benefits
- Advanced APMs – Require certified EHR, quality-based payments, and financial risk
Transition Timeline:
- Higher conversion factor on the PFS for Qualifying Participants (QPs)
- QPs receive Exemption from MIPS reporting for Advanced APMs
Value-Based Care: Opportunities Ahead
Value-Based Care continues to expand across Medicare and commercial payers.
AdvancedMD supports your transition with tools like:
- Integrated RAF Score
- EHR Patient Reporting
- HealthWatcher Reminder


Simplified Data Collection
AdvancedMD makes quality reporting easier with integrated tools for multiple reporting methods:
Certified eCQM Reporting
- ONC-certified templates for all patient populations
- Automated dashboards and scheduled reports
- Drill-down views to close care gaps
- QRDA I & III files for CMS attestation
Qualified Registry Reporting
- Access 150+ measures via Population Health Registry
- Collect MIPS CQM data using PM or EHR workflows
- Direct CMS attestation and care gap report cards
Claims-Based Reporting
- Available for practices with ≤15 clinicians
- Submit HCPCS codes for Medicare claims
- CMS tracks your Quality score
Promoting Interoperability & Improvement Activities
Value-Based Care continues to expand across Medicare and commercial payers.
Promoting Interoperability:
- Certified EHR
- ePrescribing & EPCS
- Health Information Exchange (CIE, RLE)
- Electronic Case Reporting
- Immunization Registry Reporting
Improvement Activities:
- Real-Time Prescription Benefits
- Medication Reconciliation
- Patient Forms & Portal Messaging
- HealthWatcher for proactive care

Health IT Standards
-----------------------------------------
Your Guide to MACRA & MIPS
Meaningful Use helped hundreds of thousands of independent physicians afford adding EHR to their practices. Since 2015, much has changed. The primary goal with MACRA is to improve care for Medicare patients. MACRA shifts the payment system from volume to value and results.
As an ONC 2015 Cures Update Certified EHR, AdvancedMD software meets and satisfies all the MACRA-related requirements. MACRA (Medicare Access and CHIP Reauthorization Act of 2015) introduced a new value-based reimbursement system called the Quality Payment Program (QPP) with three important changes impacting your Medicare payments.
MIPS/APMs
Created a new framework for rewarding physicians for providing higher quality care. The two tracks of the QPP are:
- Merit-based Incentive Payment System (MIPS)
- Alternative Payment Models (APMs)
SGR
Repealed the Medicare sustainable growth rate (SGR) formula that calculated payment cuts for physicians
Consolidates
Parts of three previous individual reporting programs are combined into a single system:
- Physician Quality Reporting System (PQRS)
- Value-Based Payment Modifier (VBPM)
- Medicare’s Meaningful Use (MU)
Clinical Quality Reporting (CQR)
Robust tracking software & tools help eligible professionals (EPs) easily monitor your Electronic Clinical Quality Measures (eCQMs).
Free Client Resources
AdvancedMD includes eCQM Measures as part of the monthly subscription to EHR.
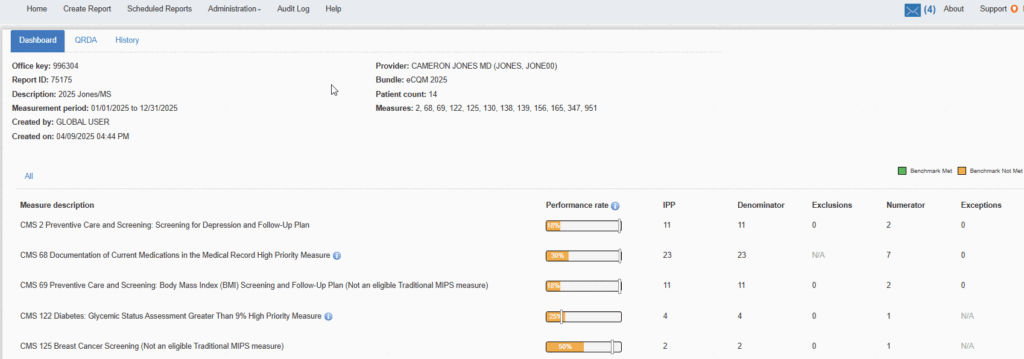
Performance Dashboard
Quickly and easily see your key physician performance indicators including rate, numerators, denominators, exclusions and exceptions.
Drilldown Information
Get a detailed view of patient summaries with flagged items that alert you of action required to improve your scores.
Scheduled Reports
Scheduled Reports to run weekly or monthly for the calendar year.
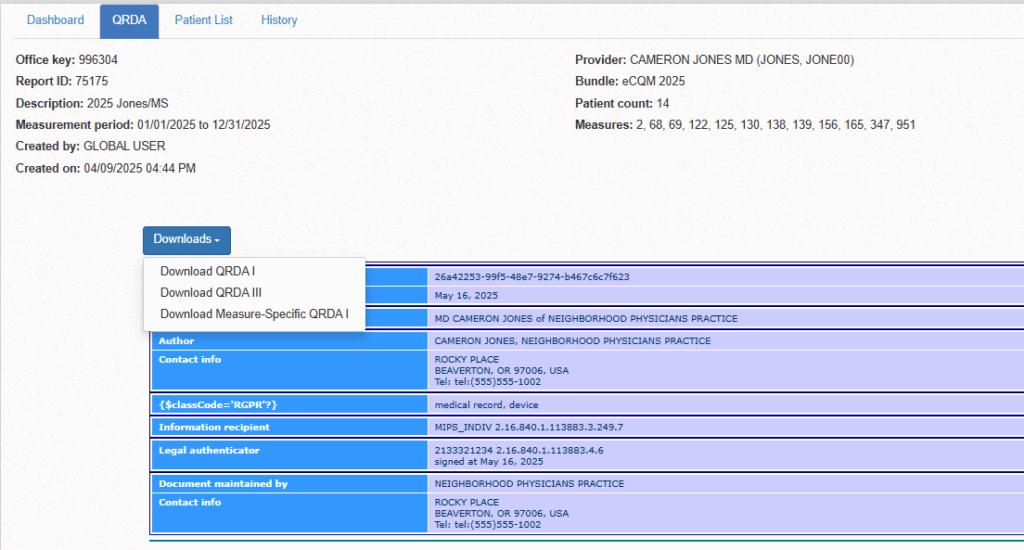
Automated Reporting
All information is QRDA III-formatted and can be submitted directly to CMS.
Professional Services
AdvancedMD offers personalized MACRA/MIPS training, consulting services to assist in you.
Why do practices find AdvancedMD eCQMs so easy to use?
Automation presents information into our intuitive dashboard, giving you a highly simplified way to succeed with CMS Quality incentives.
Intuitive dashboard that populates your most up-to-date information automatically.
We build the most flexible and user-friendly management tools available in our medical billing, health records and patient engagement technologies. Because Quality measures can seem complicated, we designed an intuitive tracking and monitoring process. AdvancedMD CQR gives you specific clinical information that is neatly organized into a simple dashboard. Information is captured automatically as you document visits in the EHR and Mobile software.
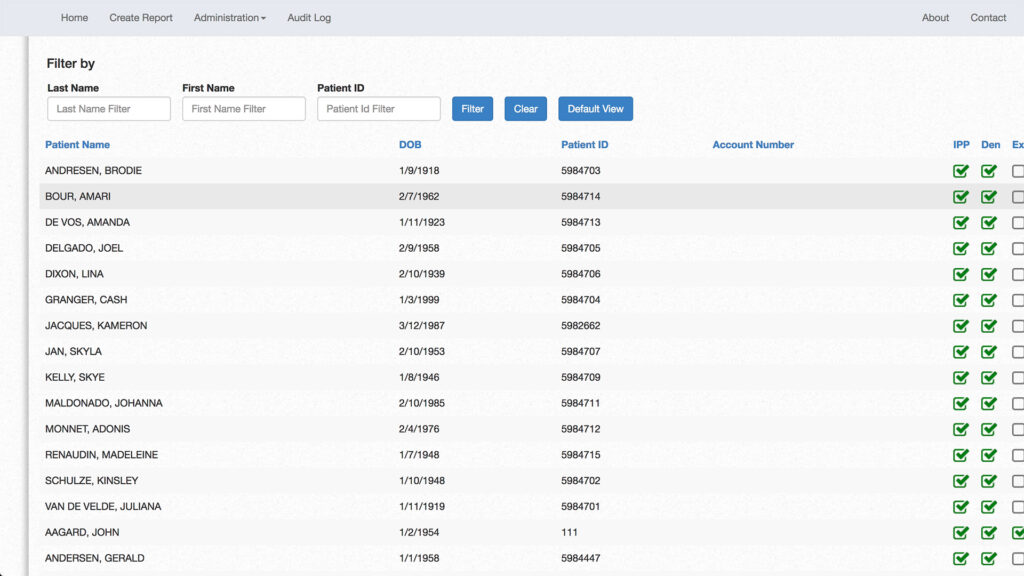
Detailed patient lists and robust reporting help you track your progress.
We designed reports – such as this patient list – that can help you understand how well you are delivering effective, safe, efficient, patient-centered, equitable and timely care. Our reports can be sent electronically to registries, such as CMS. You can also print reports for distribution within your organization. CQR is expandable and can quickly adapt to ongoing regulatory changes. CQR within the EHR is transformational because intelligent automation eliminates manual, labor-intensive steps associated with requirements for electronic clinical quality measures.
Detailed drilldowns and details help you identify performance gaps and better gauge your overall status.
Various tabs on the screen, such as “Patient Lists”, organize information in ways you can easily access and understand. Our “Drilldown” tab lets you click any line item to see your current status, including items that have been met and tips to fix those that have not. Here you can evaluate your overall progress by patient as well as your initial patient population. You can further see your overall progress and complete details that we’ve consolidated into a convenient “Details” tab.
Request a Live Demo
Complete the form below for a live demo to see all that AdvancedMD has to offer.
