Be hyper-focused on what to do next. You get a schedule snapshot and task donuts showing work volume along with critical items prioritizing what elements are most critical. It’s like having an automated workflow analyst consolidating all the moving parts of your practice.
EHR Software System Unlike Any Other
Electronic health records software with prioritized task donuts, patient cards and physician dashboard to unify all roles of your practice to improve clinical care while creating a more personal experience with patients.

The efficient EHR & EMR dashboard that’s remarkably Smart.
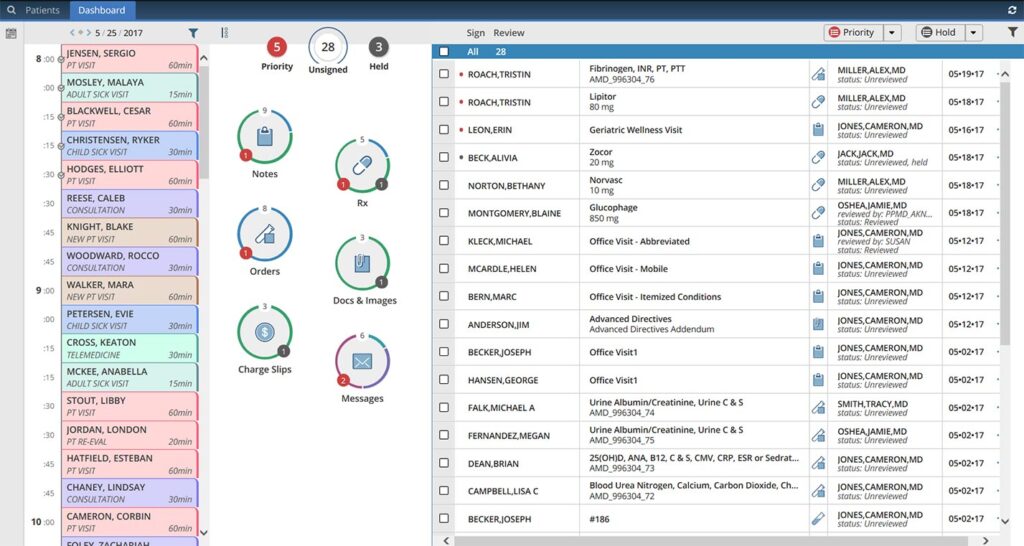
Scheduling Snapshot
Interact with your color-coded schedule and track patient rooming.
Prioritized Tasks
See your outstanding tasks in real-time, plus urgent and critical issues.
Patient Information
Quickly access common charting elements with simple summaries.
Explore EHR software features & capabilities.
All of our EHR technologies, along with our billing and patient engagement solutions, work together harmoniously. We help align every role of the practice with the right information at the right time.
EHR Dashboard
Quickly reference and access schedules, rooming, prioritized tasks, action items and patient cards.
Patient Cards
Chronologically-ordered patient information of frequent tasks to access and manage charts faster.
Task Donuts
Stay focused on work volume, view outstanding and critical tasks, and stay abreast of what to do next.
Patient Rooming
Track patient status, get wait notifications and activity metrics, while maximizing physician facetime.
Unified with Practice Management
Schedules, demographics and charges are synchronized and automatically flow bidirectionally.
Unified with Patient Tools
Engage patients with many self-service features that automatically sync with your medical records.
Customizable Templates
Gain charting productivity with flexible with note & sub-note templates designed by physicians.
Telehealth
Attract new patients, expand care to rural areas and chronic patients – while decreasing costs for all.
ePrescribing
Manage requests and renewals, and access medical histories from anywhere – even from your phone.
EPCS
Prescribe & track Schedule II-IV narcotics and electronically send to the patient’s pharmacy.
Mobile EHR iOS App
Access all your practice information on-the-go from anywhere, at anytime, in a secure environment.
Immunization Reporting
A simple way to electronically and effortlessly send patient immunization information to state registries.
Patient Health Management
Customize healthcare plans to manage conditions based on age, sex, lab results & diagnosis.
Paperless Fax
Manage information quickly and securely by converting a manual fax process to paperless.
Cloud EHR Software & Data
Enjoy an all-in-one, high-tech platform with HIPAA security, offsite storage and automatic data backup.
Multi-specialty Support
As an MSO, IPA or ACO, offer EHR to any/all physicians and manage operations as a single business.
Patient Messaging
Communicate to patients with group and personalized messages to improve relationships and revenue.
Physician Dashboard
Personalize your dashboard to track daily tasks, appointments, priority items and staff communications.
CQM Reporting
Engage in any value-based care program, maximize your scores & ultimately your reimbursement.
MACRA & MIPS
Take advantage of daily reports to know where you stand and stay ahead of required measures.
Meaningful Use
It’s not dead yet, but we will maintain compliance certification so you can successfully attest.
High-priority Checkbox
Flag high priority items in notes, prescriptions, orders, results, documents, uploads and charge slips.
Frequently Asked Questions regarding implementation of the AdvancedMD open API for integration solutions
Unable to find an answer you’re looking for? No problem. Chat with a live person and we’ll work to get your question answered.
What is EHR / EMR software?
EHR / EMR software is a computer system that helps healthcare providers manage patient medical records and automate clinical workflows. EHR systems allow providers to:
- Create customizable templates for taking notes during patient encounters
- Generate reports on practice efficiency and compliance with government programs
- Communicate with patients and staff
- See patients remotely with telemedicine sessions and prescribe medications electronically
- Sync information with practice management and billing systems
While the terms EHR (electronic health records) and EMR (electronic medical records) are often used interchangeably, they have slightly different meanings. The primary difference is that EHR puts forth the notion of interoperability, or interfacing with other medical systems to create a comprehensive view of a patient’s clinical information.
Electronic medical records represent a huge improvement over the paper-based methods of the past, and open the door to a new world of functionality for healthcare providers. As opposed to first generation EHRs that simply digitized and stored medical records, modern EHR systems act as virtual assistants that organize and prioritize practice workflow. As EHR technology continues to evolve, providers will be able to connect with patients in more meaningful ways and continuously provide better care.
How can an EHR system benefit a private practice?
Using an EHR system can significantly impact a medical practice’s bottom line. Specific benefits of EHR software include:
- Saving time by automating manual processes like charting and prescribing medications
- Streamlining physician workflows with scheduling, task prioritization, and communication tools
- Protecting against data breaches and ensuring HIPAA compliance with increased PHI (protected health information) security measures
- Accessing patient records from anywhere using mobile devices
- Reporting functionality that helps providers participate in government-run EHR Incentive Programs.
Another benefit of modern EHR systems is seamless integration with practice management software. This integration eliminates time and errors caused by copying-and-pasting between software systems, reduces the amount of missed follow-up appointments, and speeds up reimbursement.
The cumulative result of these benefits is a medical practice that runs more efficiently, allowing providers and office staff to focus on caring for patients and maintaining profitability.
How does an EHR improve the quality of care for patients?
To be able to provide the best care possible, healthcare professionals need to be able to quickly understand patient histories and maintain efficient ongoing communication with patients about their health and treatment plans.
EHR / EMR software allows providers to use note templates that capture relevant information during patient encounters, and to quickly recall this information as needed. As interoperability between medical information systems becomes more commonplace, patient records are more accessible along the entire care continuum. For instance, having easy access to a patient’s medical history can dramatically improve the quality of care they receive during a visit to the emergency room, when time is of the essence.
In addition to making records more accessible, modern EHRs can help providers significantly reduce mistakes, especially when prescribing medications.
EHR systems also improve the communication channel between providers and patients. For example, the EHR system can integrate with scheduling systems to automatically remind patients of upcoming appointments. Then providers can use patient portals to securely communicate treatment plans, prescription instructions, and other helpful information to patients.
Alongside patient portals, the emergence of telemedicine is making healthcare even easier for patients. Telemedicine sessions allow providers to diagnose and treat patients over the phone or via video chat. Patients can benefit from medical advice from the comfort of their own homes, and save time and money that would have been spent on travel.
How much does an EHR system cost?
The cost of most EHR systems depends on the number of providers using the software and/or the number of patient encounters per month. Additional functionality, such as e-prescribing for controlled substances and lab integrations, can also affect price.
Our pricing is flexible and designed to make sure you get exactly what you need for the most affordable price. We offer both per-provider and per-encounter plans. Visit our pricing page to find a plan that best fits your business.
What is a “certified EHR?”
A “certified EHR technology” (CEHRT) is an EHR/EMR system that has been reviewed, tested, and certified for use in incentive and compliance programs administered by CMS.
The goal of the EHR Incentive Programs, recently renamed the Promoting Interoperability (PI) Programs, is to encourage providers to use EHR / EMR software and to help them find technology that meets program requirements. These programs offer incentives to healthcare providers that use a certified EHR and impose penalties on those who don’t meet standard requirements.
For instance, one measure that can contribute to a medical practice receiving an incentive payment is demonstrating that a certain percentage of their patients actively use a patient portal.
As EHR vendors develop new technology, they submit it to an ONC-ATCB (ONC-Authorized Testing and Certification Body) for inspection and testing. After receiving certification, the ONC-ATCB monitors the technology for continued compliance.
AdvancedMD v12.7 is 2015 Edition compliant and has been certified by an ONC-ACB in accordance with the applicable certification criteria adopted by the Secretary of Health and Human Services. This certification does not represent an endorsement by the U.S. Department of Health and Human Services.
Request a Live Demo
Complete the form below for a live demo to see all that AdvancedMD has to offer.
