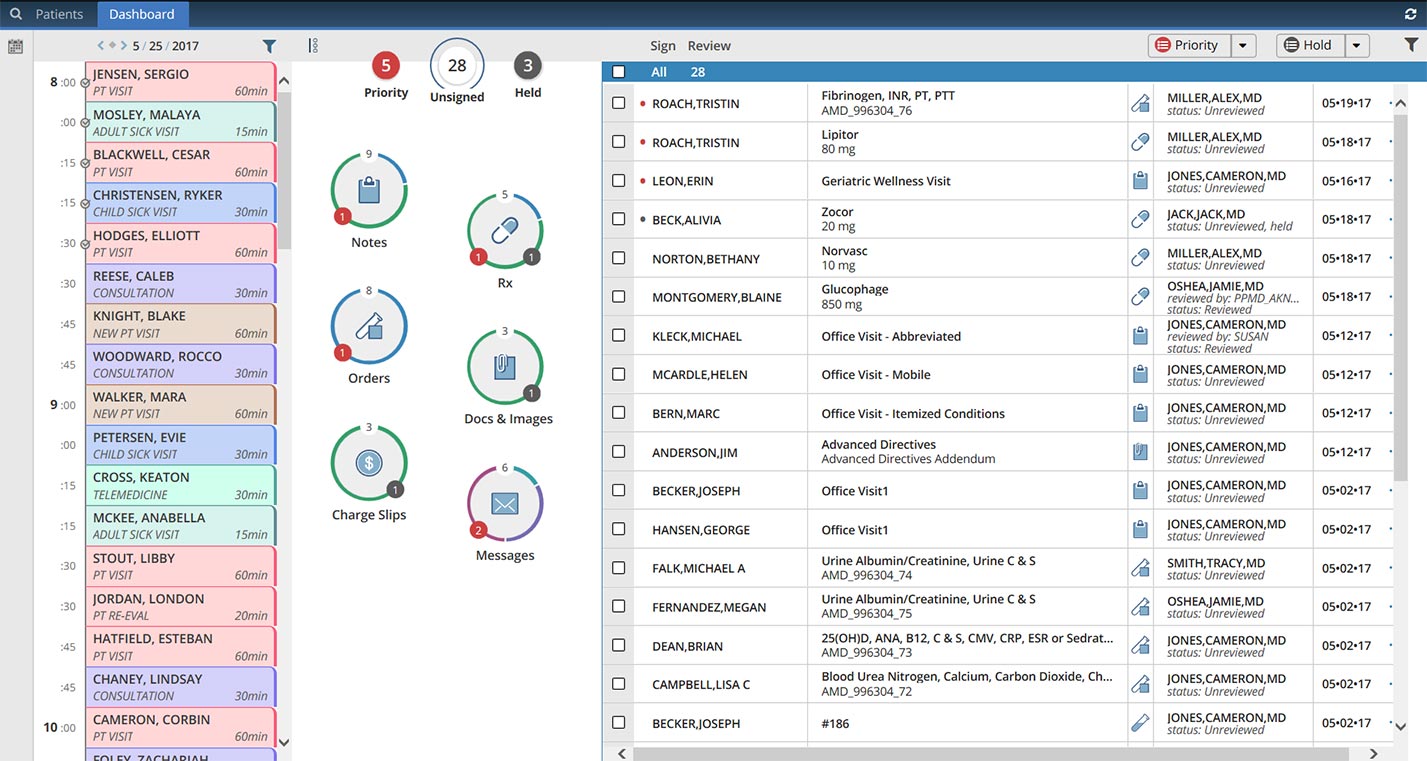
A “certified EHR technology” (CEHRT) is an EHR/EMR system that has been reviewed, tested, and certified for use in incentive and compliance programs administered by CMS.
The goal of the EHR Incentive Programs, recently renamed the Promoting Interoperability (PI) Programs, is to encourage providers to use EHR / EMR software and to help them find technology that meets program requirements. These programs offer incentives to healthcare providers that use a certified EHR and impose penalties on those who don’t meet standard requirements.
For instance, one measure that can contribute to a medical practice receiving an incentive payment is demonstrating that a certain percentage of their patients actively use a patient portal.
As EHR vendors develop new technology, they submit it to an ONC-ATCB (ONC-Authorized Testing and Certification Body) for inspection and testing. After receiving certification, the ONC-ATCB monitors the technology for continued compliance.
AdvancedMD v12.7 is 2015 Edition compliant and has been certified by an ONC-ACB in accordance with the applicable certification criteria adopted by the Secretary of Health and Human Services. This certification does not represent an endorsement by the U.S. Department of Health and Human Services.